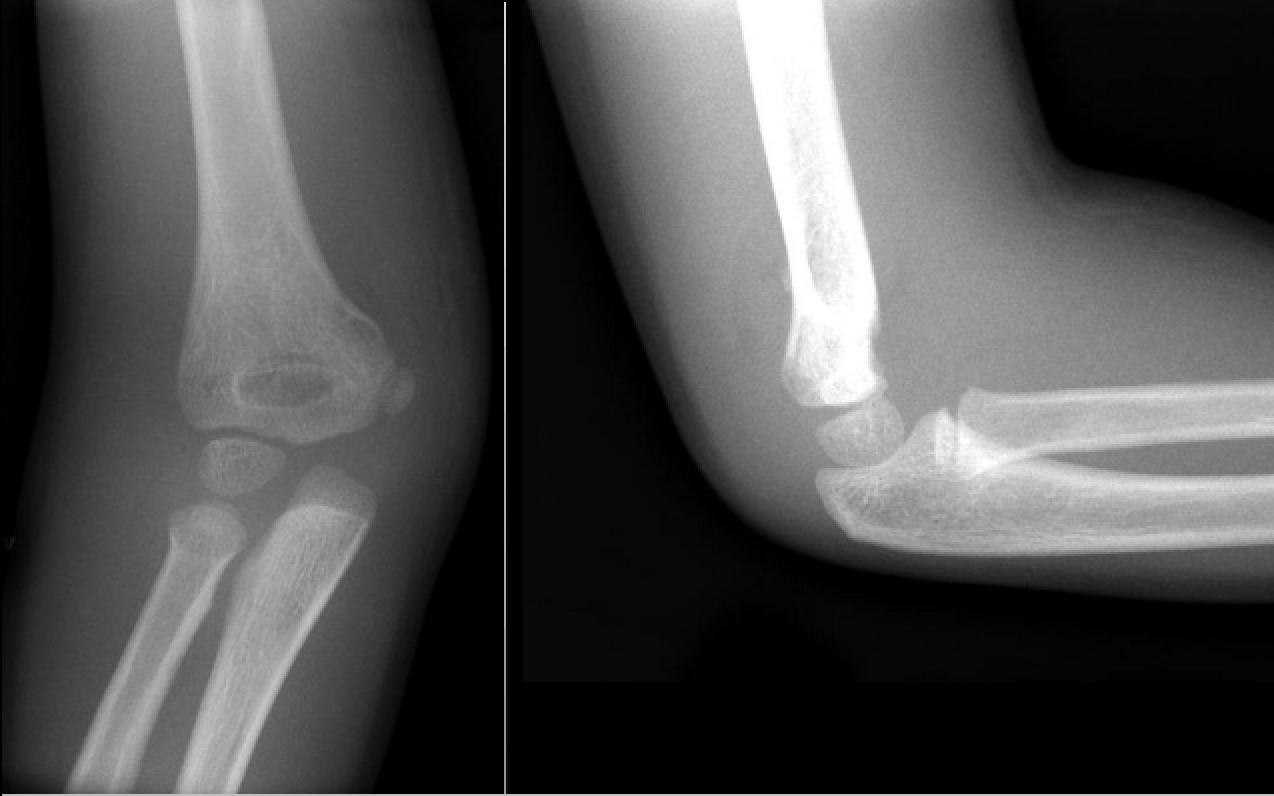
Specific reasons for extended immobilization included the following: unknown reason 75/389 (19.28 %), early pin removal 1/389 (0.26 %), pain/tenderness 3/389 (0.77 %), family or physician concern due to an active child 3/389 (0.77 %), and surgeon interpretation of delayed healing from radiographs 4/389 (1.03 %). Following pin removal, 86/389 (22 %) patients were immobilized for additional time (1–4 weeks). The only intervention encountered after pin removal was extending immobilization in cast. The median of number of radiographs following pin removal for these 119 patients was two (range 2–12). Of 389 patients, 119 (31 %) had radiographs taken after day of pin removal during follow-up visits. 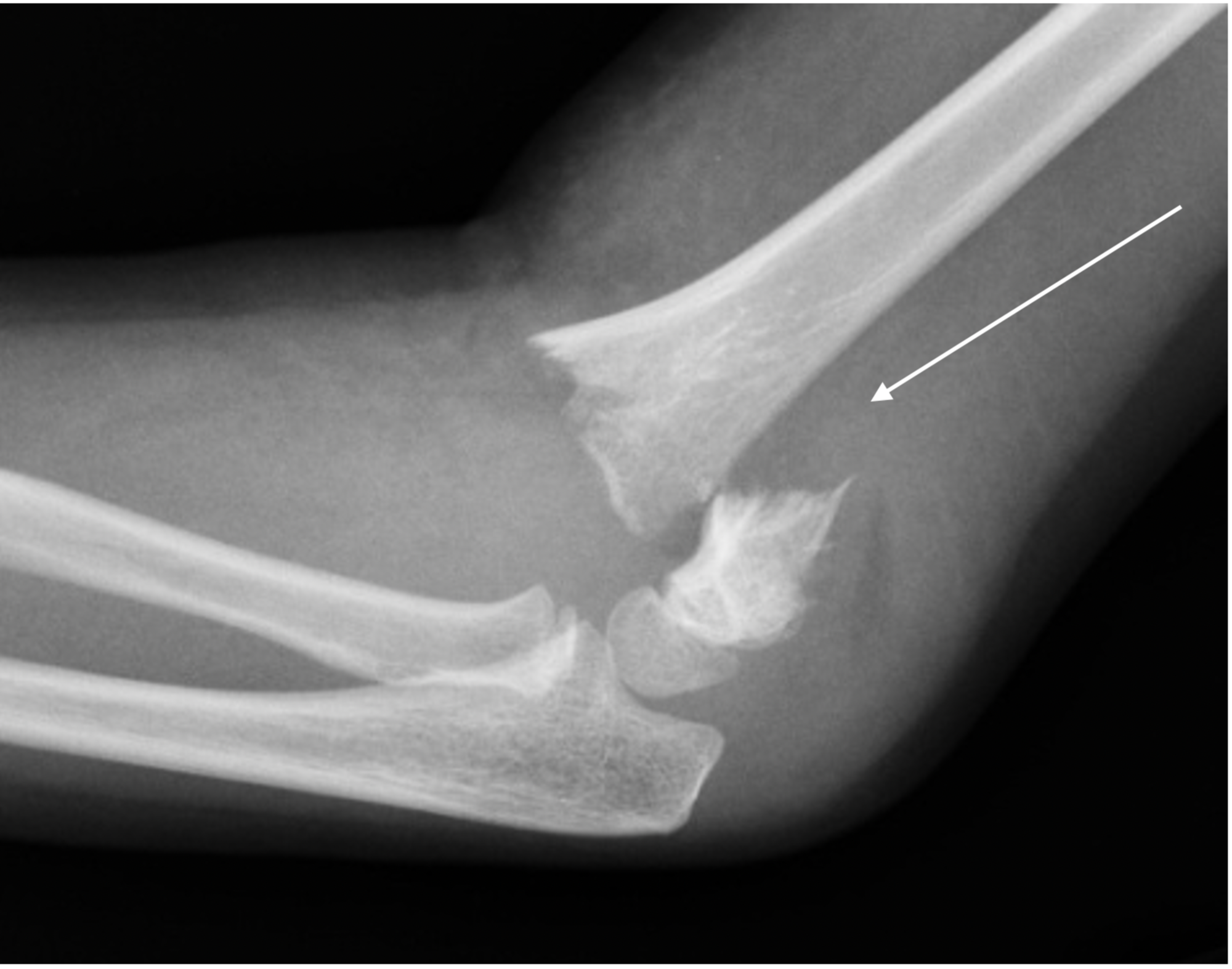 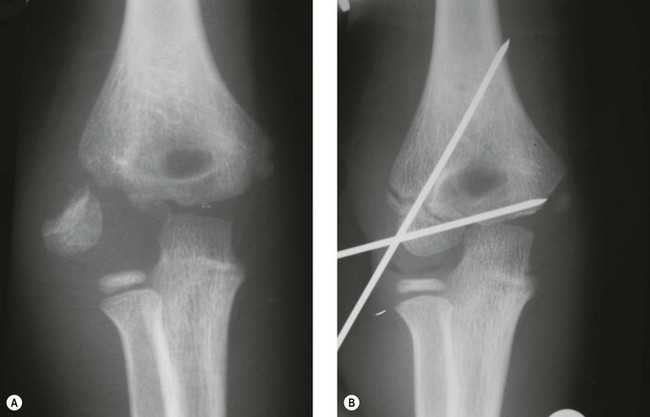
The median number of total post-operative radiographs taken was four (range 2–14) while the median number of radiographs taken on day of pin removal was two (range 2–4). A two-sided binomial test was used to test the null hypothesis that the proportion of subjects that underwent intervention secondary to radiographic findings was equal to 5 %. All were de-identified prior to review by the senior author.ĭescriptive statistics were used to summarize the proportion of subjects that underwent additional interventions after pin removal and the reason(s) for the interventions. The senior author was a surgeon for patients in the cohort and assisted with radiographic review in selected cases. The lead author reviewed all images and was not involved in patient care for this population. Visible fracture callus adjacent to the cortices on both frontal and lateral views was considered appropriate fracture healing. Radiographs at day of pin removal and radiographs taken at any subsequent visits were compared to pre-operative and intra-operative imaging to discern loss of fracture reduction and the presence of fracture healing. Additional intervention after pin removal due to radiographic findings was the primary outcome variable of interest. Follow-up after pin removal is on an as needed basis. In general, first post-operative follow-up occurs 2–3 weeks after surgery for pin removal. They had varied regimens in terms of need for casting after pin removal and number of visits scheduled after pin removal. Eighteen surgeons were included in the study cohort. Early pin removal is defined as pins removed earlier than planned at time of surgery. Study data were retrospectively collected including demographics (age and gender), surgical characteristics (attending surgeon, number of pins, pin configuration, and pin size), and post-operative clinical characteristics (days to pin removal, if pin removal was early or delayed, neurologic complication, vascular complication, surgical site infection, re-fracture after pin removal, loss of reduction on radiographs at pin removal and at subsequent visits, total number of radiographs taken post-operatively). We hypothesized that the interventions at time of pin removal based on radiographic findings would be rare. The purpose of this study was to evaluate the utility of post-operative radiographs taken at time of pin removal for patients healing uneventfully after CRPP of a type 2 supracondylar humerus fracture. Two studies have suggested that radiographs after surgical treatment but prior to planned pin removal do not alter management. Recent literature has demonstrated an interest in reducing the instances of unnecessary radiographs. Prior studies have demonstrated extremely low rates of loss of reduction or implant failure in patients with supracondylar humerus fractures treated by CRPP. Intra-operative fluoroscopy is routinely used to assess fracture reduction and verify appropriate divergent placement of percutaneous pins. This management strategy has low rates of malunion, nerve injury, vascular injury, or compartment syndrome in patients and avoids the high rate of loss of reduction observed with non-operative care. At our institution, type 2 supracondylar humerus fractures are almost exclusively treated operatively with closed reduction and percutaneous pinning (CRPP).
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
